Clinician library · progress
What does progress mean?
Progress is often messy, circular, and subtle. Here are five shifts many therapists watch for—especially early on.
Therapists care deeply about clinical momentum. They want to know:
- Did the patient remember what we talked about last week?
- Are we actually making progress, or are we starting from scratch every Tuesday?
- Does the technology get in the way of the human connection?
If I had to compress therapy's big-picture goals to #1 and #2:
#1: Reduce suffering and improve real-life functioning. Not just "feel better in session," but sleep, work, relationships, conflict, self-trust, and day-to-day choices getting better outside the room.
#2: Build durable inner capacity so change lasts. Clients become better at noticing, naming, regulating, and communicating their inner experience under pressure, so they rely less on crisis patterns over time.
What therapists are usually hoping to see as outcomes:
- Short-term: less overwhelm, less shutdown/avoidance, better contact with what the client is actually feeling.
- Mid-term: better emotional differentiation, better regulation, better conversations/repairs in relationships.
- Long-term: more agency, values-aligned behavior, fewer relapse loops, and progress that generalizes beyond therapy.
A useful litmus test: therapists care less about "insight as a concept" and more about clinically usable movement week to week.
In therapy, progress is rarely a straight line upward. It often shows up as a few small, specific shifts that change what becomes possible—inside the session, and in the client’s real life.
Every therapist has their own style and theory of change. But across modalities, many clinicians are listening for the same kinds of markers: more awareness, more capacity, and a clearer relationship to the self.
What progress can look like in therapy
- More access: the client can contact what’s happening internally (even briefly) instead of going blank, intellectualizing, or getting hijacked.
- More tolerance: they can stay with experience a little longer without flooding/shutdown/escape.
- More choice: a wider gap appears between impulse and action.
- More integration: experiences link up (body ↔ emotion ↔ meaning ↔ need ↔ action) with less fragmentation.
- More relational freedom: old patterns show up, get named, and become negotiable—especially in the room.
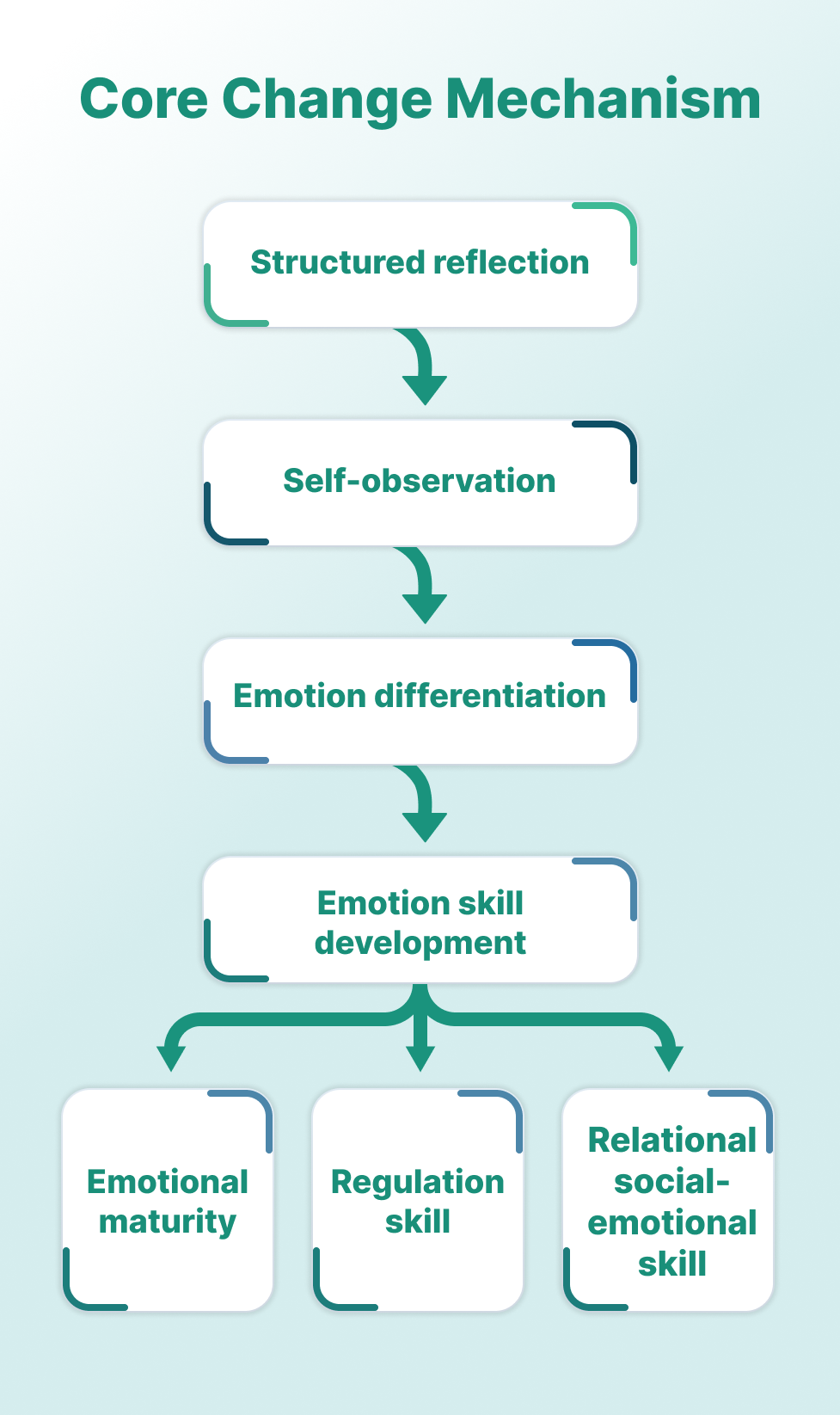
Progress signals
Five things therapists often care about
These are not “grades.” They are the kinds of shifts that help the work move from surviving to thriving.
1) Increased self-awareness (the “aha” moments)
- Connect the dots: “I realized I get angry at my partner because it reminds me of how my dad used to dismiss me.”
- Identify triggers: naming what sent you into a spiral instead of only feeling ‘bad.’
- Notice body signals: “My chest tightens right before I say yes to something I actually want to refuse.”
2) Emotional regulation and resilience
- Shortening the refractory period: if a panic spike used to ruin a week and now it ruins an afternoon, that’s a major win.
- Expanding the window of tolerance: staying in a hard topic without shutting down or exploding.
- Self-soothing: using grounding, breath, or another tool without being prompted.
3) Shifts in internal dialogue
- The inner critic softens: moving from “I’m a failure” to “I made a mistake, and I’m human.”
- More ownership and agency: moving from “Everyone makes me miserable” to “I notice I feel miserable in these environments—and I can choose what I do next.”
4) Behavioral changes (the real‑world test)
- Setting boundaries: saying no to an overreaching boss or a harmful family pattern.
- Breaking cycles: choosing a healthier partner, or reaching for a journal instead of a bottle.
- Behavioral activation: doing the hard thing even when you do not feel like it (e.g., going for a walk while depressed).
5) The quality of the therapeutic alliance
- Disclosing “the secret”: sharing the thing that felt too shameful to say in month one.
- Challenging the therapist: “I didn’t like what you said last week” can be a sign the relationship is safe enough for healthy conflict.
A note on “small” wins
Therapists often care most about the progress a client is most likely to dismiss. Getting out of bed and showering during a depressive episode can represent an enormous amount of effort and capacity.
In many cases, the win is not “feeling good.” The win is staying connected, staying curious, and showing up—especially when every part of the system wants to shut down or cancel.
The gold standard
Progress is defined by the client’s goals.
If someone came in to stop having nightmares and the nightmares stop, that’s the progress that matters.
Practical
A simple list to bring to your next session
If you want more structure, here are a few “progress markers” you can use as prompts in session—without turning therapy into a performance.
Awareness
- What are the earliest signs I’m getting activated (body, thoughts, urges)?
- What were the exact triggers, and what did they mean to me?
- What am I avoiding naming?
Regulation
- How long does it take me to come back after I spike or shut down?
- What helps me return to the room (grounding, breath, movement, connection)?
- What is one “smaller” version of the hard thing I can do this week?
Further reading: What are emotion skills? and Why naming our emotions matters.
A clinician lens
The markers I personally watch for (session-to-session)
These are the “small, specific” shifts that often predict bigger change later—without requiring a client to feel good yet.
- Shift from global to specific: “Bad” becomes “hurt + ashamed + angry,” or “anxious” becomes “anticipatory dread + embarrassment.” Specificity predicts options.
- Earlier noticing: they catch the wave at the beginning, not after the rupture/blow-up/binge/avoidance.
- Shorter recovery time: not “never dysregulated,” but “returns sooner” and “with less collateral damage.”
- New responses under stress: not just doing well on good days—doing one different thing when activated.
- More accurate ownership without self-blame: “This is my pattern” and “I’m not a bad person for having it.”
- More honest contact in the alliance: rupture/repair, disagreement, disappointment, saying the unsayable—without punishment or withdrawal.
- More agency in micro-decisions: boundary-setting is one form; another is choosing pacing, asking for clarification, naming confusion, pausing.
- Generalization: the skill appears outside the session (even once) and then starts to repeat.
How can Feelpath Support Emotion Work
Feelpath supports emotion work by making emotional capacity changes easier to notice and easier to build on. In many clients, the first wins aren’t dramatic insights—they’re small shifts in access and tolerance: staying with experience a few seconds longer, noticing earlier, moving from “I feel bad” language to specific emotion words that can guide action, and finding a workable link between body cues and meaning.
Feelpath supports emotion work by protecting the relational core while strengthening the client’s access to inner experience. Early progress often isn’t “insight” or “behavior change” yet—it’s a client who can notice sooner, name more specifically, and stay present a little longer without escaping into facts, jokes, or shutdown. That’s not just language; it’s capacity.
In session, Feelpath helps you lower the performance demand. Instead of the client having to invent the perfect word on the spot, you can support recognition and differentiation while staying attuned. That keeps shame low and collaboration high, which is often the condition for the work.
In session, Feelpath helps you reduce the demand to produce the right word under pressure. By lowering cognitive load, you can keep the relational work primary while still giving the client a concrete path from cue → feeling → meaning → need. The point isn’t perfect labeling; it’s steady practice that makes choice possible.
Across weeks, it helps you noticed clearer evidence: what’s becoming more differentiated, what’s being noticed earlier, where recovery time is shortening, and where the client is starting to respond differently under stress. That’s the kind of progress that tells you the work is taking.
Feelpath supports emotion work by giving me better visibility into the progress I actually care about: emotional access, emotional tolerance, and emotional choice. I don’t need a score. I need to see whether my client is getting closer to their internal experience, whether they can stay with it longer without shutting down or flooding, and whether a little more space is opening up between impulse and action.
The goal is to help the client build usable links: body cue → felt sense → emotion → meaning → need → next step, at a tolerable pace. Across weeks, progress becomes more visible in the ways that matter clinically: more differentiation, steadier tolerance, shorter recovery time, and emerging choice under stress. When those signals show up, you can feel more confident about where to deepen, where to slow down, and what to return to next.
A guiding frame
Change requires contact with felt meaning.
So the clinician needs tools that make it easier to:
- Get to the experience (recognition > generation, cue → label → meaning).
- Hold onto it across sessions (so there’s a thread to return to and build on).
- Notice capacity-based progress (not “better mood,” but more differentiation, earlier noticing, more tolerance, emerging choice).
